分析临床病例,锻炼医学英语实践能力。
by John Burton, M.D.
A 90-year-old woman has been a patient of the Beacham Ambulatory Care Center since 2000. Chronic conditions are pernicious anemia, osteoarthritis, and urinary incontinency. She is fully functional and fully independent. She provides care for the homebound husband who has severe COPD. They live in a row home specifically “close to the hospital” to ensure access to house calls for her husband.
In September 2000, the husband dies as a result of respiratory arrest. Her only relative is a nephew who talks with her about once a month. In October 2002, her home is broken into and our patient is raped and robbed. She was taken to a local hospital specializing in rape. Here, she is distressed, delusional, and is reported to be very emotionally distraught.
We see the patient about 3 weeks after the rape in a community nursing home, where she was moved after a 4 day stay at the hospital. She was very distressed, delusional and confused. She slowly improved over 2 months and was discharged to a senior living building in a community in eastern Baltimore County.
In March of 2003, the patient is seen in the office. She is still very ill emotionally. She is crying, depressed (not suicidal), and stressed about her new home. She wants to move to a new Senior Housing unit because it would be on the bus route making it easier to get around. She has also hired a middle aged woman as a caregiver.
In November 2003, 9 months after moving to a new facility, she becomes acutely ill with psychotic symptoms and severe paranoia. She hallucinates that men and women are in her bed and calls others all hours of the day. She is hospitalized on a psychiatric unit and improves over about 14 days without antipsychotic medication.
One week following discharge from the hospital, symptoms rapidly recurred when she returned to the senior apartment. She was disruptive and threatened with eviction unless something was done rapidly. An emergency petition was prepared as she refused medical care. With the help of her companion, we were finally able to persuade her to take a neuroleptic drug (Haloperidol 0.025 – 1.0 mg/day) for her recurrent incapacitating hallucinations. Our office nurse and staff called her daily to guide her through the process of taking her medicines. She slowly but steadily improved and became stabilized.
Post Traumatic Stress Disorder
Basic Facts on Elder Rape
The graph below indicates the increase in elder abuse reports since 1986.
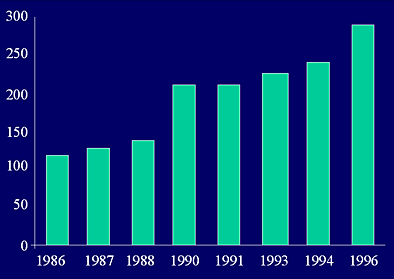
Reference: Tatara, Toshio and Lisa Kuzmeskus. Summaries of Statistical Data on Elder Abuse in Domestic Settings for FY 95 and FY96. (Washington, DC: National Center on Elder Abuse, 1997)
PTSD is a serious disorder that results from exposure to a traumatic event. The concept was formulated during the Vietnam War. An event is considered traumatic if it is extreme, death threatening or causes serious injury, and the response involves severe fear, helplessness and horror. Clearly our patient experienced a major traumatic event.
Examples of Traumatic Events in the Elderly
PTSD occurs relatively commonly in elderly patients (13% - Psychother Psychosom 2003) compared to 10% in the general population. Prevalence is higher in Holocaust survivors, in patients with cancer, and in patients following heart surgery.
There are 3 cardinal symptom categories; 1) re-experiencing the event, 2) avoidance and numbing, and 3) increased arousal. *
1. Re-experiencing the event (1 must be present)
2. Avoidance/Numbing (3 must be present)
3. Increased Arousal (2 must be present)
Classification of PTSD is based on the duration of symptoms. *
| Acute Stress Disorder | < 1 month |
Acuted PTSD | 1-3 months |
Chronic PTSD | > 3 months |
| *Culpepper; Primary Care Companion Reports 2003 | |
Additionally, other psychological symptoms are often present including major depression (50% of cases), substance abuse or dependence, panic/agoraphobia.
PTSD is a treatable condition and therefore it is important to recognize. Without treatment, PTSD is disabling in 50% of cases. Slightly less than 50% of patients are untreated. Informing the patient about the illness and its course through educational counseling help patients and their families cope. Cognitive therapy (a specific form of interactive counseling) requires referral to a psychologist experienced in this form of counseling.
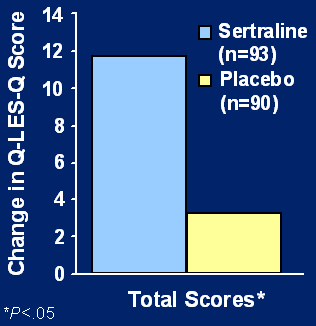
SSRIs (antidepressants) may be necessary. The graph below is from a study by Brady, etal (JAMA 2000, 283:1837) comparing the change in Q-LES-Q* scores in patients taking an SSRI, Sertraline (n=93) versus patients taking a placebo (n=90).
*Q-LES-Q (Quality of Life Enjoyment and Satisfaction Questionnaire) measures mood, social relationships, leisure time activities, ability to function in daily life, living/housing, ability to get around, and work/hobby.
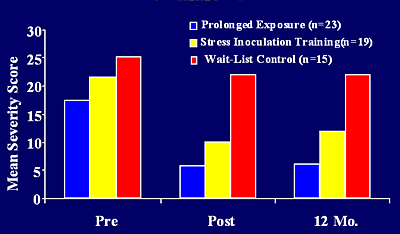
In a study by Foa E et al (J Consult Clin Psychol. 1999; 67:194-200), investigators show the benefit of cognitive counseling by a psychologist on the severity of depression measured using the Beck Depression Inventory (BDI). These results are summarized in the graph below.